Welcome to the Qualified Health Plan Website
This is the official Centers for Medicare & Medicaid Services’ website for issuers seeking certification to participate in the Federally-facilitated Exchanges (FFEs). As defined in the Affordable Care Act (ACA), a qualified health plan (QHP) is an insurance plan that is certified by the Health Insurance Marketplace, provides essential health benefits (EHBs), follows established limits on cost sharing, and meets other requirements outlined within the application process. The QHP Application, materials, and other resources are available on this site to facilitate the certification process.
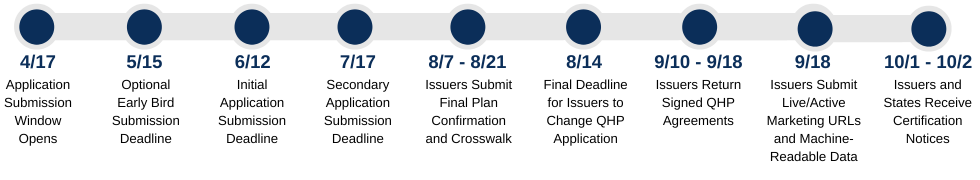 Select any of the hyperlinked icons below to access key webpages containing guidance for issuers seeking certification.
Select any of the hyperlinked icons below to access key webpages containing guidance for issuers seeking certification.
